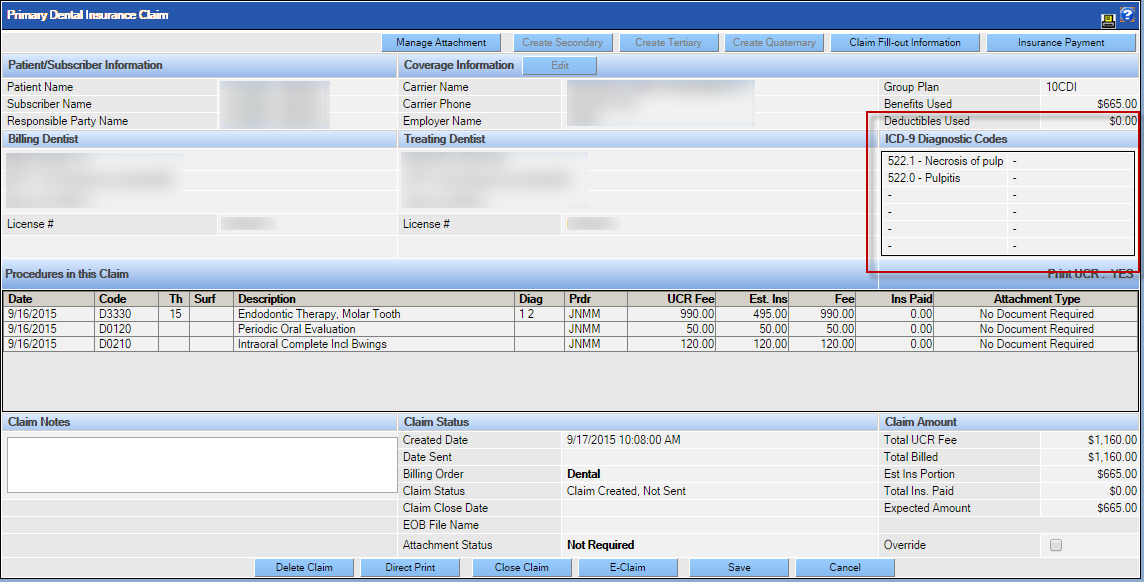
Diagnosis codes added during the clinical entry process will be included in the claim. QSIDental recommends that users dual code procedures, meaning enter both ICD-9 and ICD-10 codes during the transition period. In this way, the claim will include only the codes currently being accepted by the carrier (according to the carrier setup in QSIDental Web).
Users may refer back to the claim in QSIDental Web to see which diagnosis codes were printed or transmitted to the carrier. If the claim status is ‘Not Sent’, the codes expected to be printed are displayed, but will be reanalyzed at the time the claim is printed/e-claim created.